The thought of having a Pap Smear can be daunting, but after your first few, Pap Smears will become just like dental check ups, haircuts, waxing appointments, annual flu shots, or any other regular appointments.
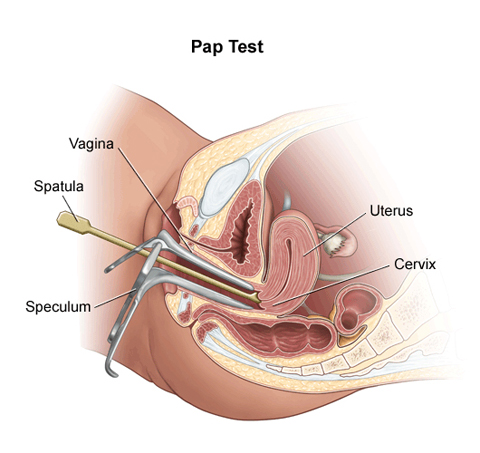
Pap Smears save lives. A Pap Smear involves testing the cells of your cervix for infection with HPV, or any cancerous or pre-cancerous changes. If pre-cancerous changes are picked up they can be easily treated, thus avoiding progression to cervical cancer.
Pap Smears are provided for free by the NHS every three years for females age 25 and over. In countries that do not have Pap Smear screening programs there are still very high rates of cervical cancer and deaths from cervical cancer. Cervical cancer is the third most common cancer in females worldwide. This is why it is so important to have your three-yearly Pap Smears. Furthermore, treating a pre-cancerous cervical lesion is much easier and less distressing than treating cervical cancer.
What causes cervical cancer?
Cervical cancer is usually caused by the Human Papilloma Virus (HPV). HPV can be contracted from touching, not just vaginal, anal, or oral sex with someone who has the virus, so even if you do not have penetrative sexual intercourse with a male, you could still have HPV and be at risk of cervical cancer.
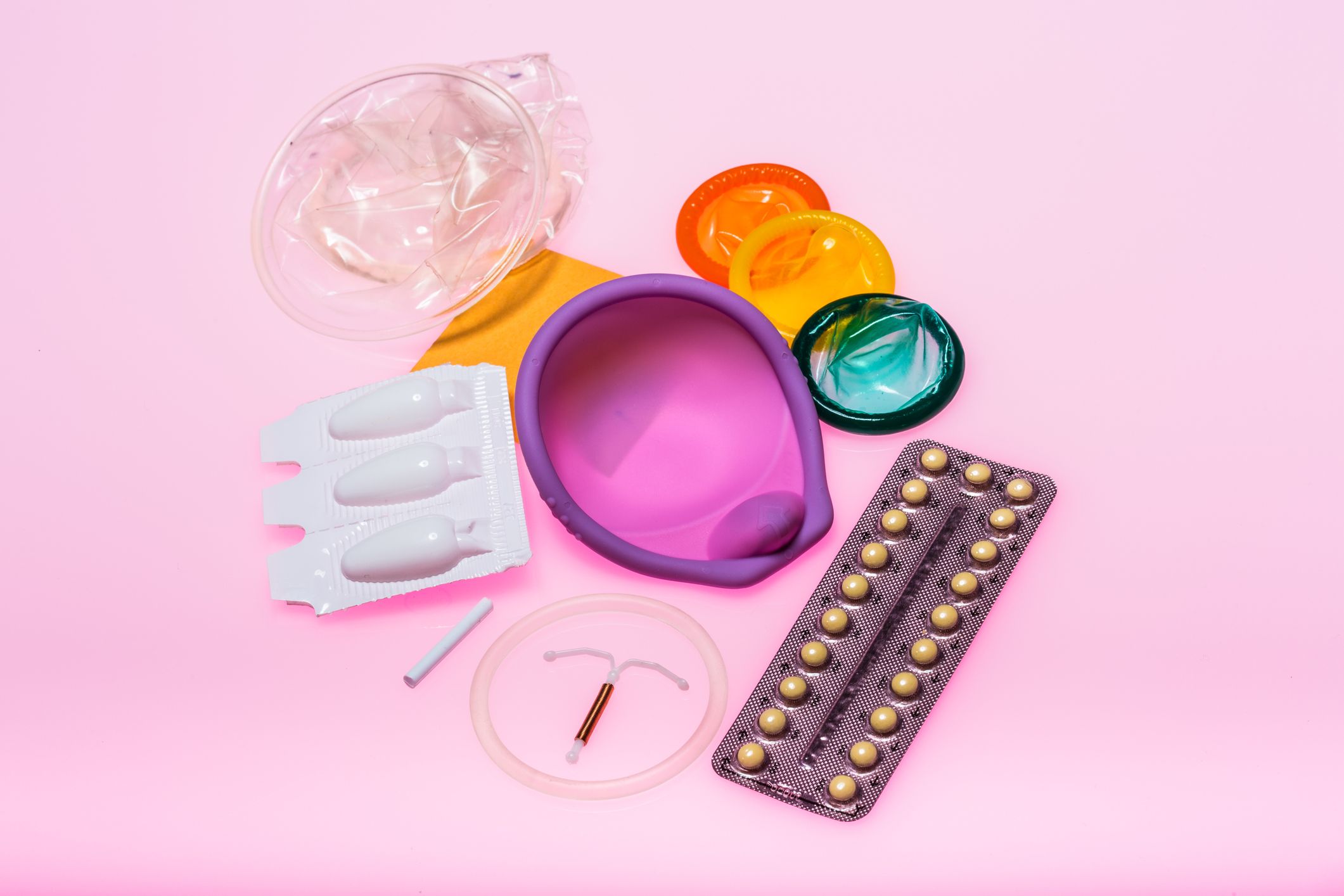
The HPV vaccine is provided free of charge on the NHS for girls aged 12-18. The best time to have the vaccine is before exposure to the HPV i.e. before becoming sexually active, which is why it is routinely given to girls aged 12-13. If you are a female aged over 18, or are male, you can still get the HPV vaccine but will have to pay full price for it. The price is roughly £130 per dose, and 2-3 doses are required.
The HPV vaccine provided in the UK also has the added benefit of protecting against genital warts which can be unsightly, uncomfortable, and sometimes cause issues like bleeding, or rarely, urinary obstruction. You can read more about the HPV vaccine here. It is important for all eligible females to have the HPV vaccine and three-yearly Pap Smears so that they can protect themselves against cervical cancer.
At the clinic
As a doctor who has performed countless Pap Smears, it is part of my everyday job, just like testing someone’s’ blood sugar level or measuring their blood pressure. If you feel nervous before you first appointment, which is completely normal, just remember that your doctor has done this many times and doesn’t care in the slightest if you haven’t shaved or waxed or what you look like “down below”. To be honest, your doctor probably won’t even notice, as they will be too focused on getting a good smear for the experts in the lab to analyse.
The first time you have a Pap Smear your doctor should go through the procedure with you and make sure you are comfortable and understand what it involves. A Pap Smear may feel uncomfortable but it should never be painful. Let your doctor know straight away if it is painful so that they can stop and figure out what is causing you pain.
Let your doctor know before the Pap Smear if you have been experiencing any concerning symptoms, like vaginal bleeding in-between periods, or pain. This is so that they can look for anything that might be causing the symptoms whilst they are performing the Pap Smear and examining you.
It is your prerogative to request a female or male doctor, or a doctor you feel most comfortable with. Doctors will not be offended if you request another doctor. We understand that this can be an awkward and embarrassing procedure for patients and our primary concern is that you feel comfortable so that you will want to continue to engage with the Pap Smear screening programme every three years and stay cervical cancer free.
The procedure
The technique doctors use may vary slightly, but this is an overview of the general 10 steps process your doctor might follow:
Step 1 – Your doctor will ask you to remove your bottoms and underwear behind a curtain and lay on the examination bed with a sheet covering yourself.
Step 2 – The doctor will either ask you to bend your knees, put your feet together, and bring your knees out, or if you are on a bed with stirrups, they will ask you to place your feet in the stirrups. This position makes it easiest for the doctor to perform the Pap Smear. The doctor might ask you to put your hands under your bottom to elevate your pelvis, again, making their job easier. If at any point you feel uncomfortable or need a break, don’t be afraid to let your doctor know.
Step 3 – The doctor will feel your abdomen for any pain or lumps.
Step 4 – They will then arrange a lamp to shine a light on your vagina so that they can get a good view. They will inspect the outside vulval area for any abnormalities.
Step 5 – They will insert a speculum slowly into the vagina. The speculum will be opened up and locked into place so that the doctor can visualise your cervix.
Step 6 – The doctor will use a small brush to collect some cells from the cervix and then coat the cells onto a slide to be sent to the laboratory.
Step 7 – The doctor may offer to take swabs for chlamydia and gonorrhoea. If so, they will need to use another brush to take some more cells and send them off for testing.
Step 8 – The speculum will be closed and slowly removed.
Step 9 – The doctor will then perform an “internal bimanual examination”. This involves inserting two fingers into the vagina and using the other hand to feel the abdomen. The doctor will feel for your ovaries and uterus, making sure there is no abnormal lumps or pain.
Step 10 – The doctor will then let you get dressed.
Results
Your results may take a week or so and they may tell you your results over the phone or in person, depending on the protocol of the clinic. If your results are normal, you should have your next Pap Smear in three years time. If your results are abnormal, your doctor will discuss with you what to do next. Abnormal results may not necessarily mean you have cancer. You may have signs of a HPV infection that requires careful observation, or a pre-cancerous lesion that may require further investigations.
A Pap Smear is different from a sexually transmitted infection (STI) test, so just because you have had an STI test, doesn’t mean you have been screened for cervical cancer. If you have had the HPV vaccine, you still need to have three-yearly Pap Smears as the vaccine does not protect against all strains of HPV, and for the strains it does protect against, it is not 100% effective. The best way to prevent cervical cancer is to get the HPV vaccine if you are in the eligible age group, and to have three-yearly Pap Smears.
If this doesn’t convince you, here is a short video explaining the impacts of HPV and why you should get tested:
[vsw id=”qvxUr3gRAa0″ source=”youtube” width=”700″ height=”500″ autoplay=”no”]
Get tested and vaccinated if you haven’t already!